A Smartphone-based Obesity Risk Assessment Application Using Wearable Technology with Personalized Activity, Calorie Expenditure and Health Profile
2 School of Innovation Design and Engineering, Mälardalen University, Sweden, Email: maria.linden@ub.uu.se
Received: 30-Aug-2019 Accepted Date: Feb 11, 2020 ; Published: 18-Feb-2020
Citation: Hosseini HG. A Smartphone-based Obesity Risk Assessment Application Using Wearable Technology with Personalized Activity, Calorie Expenditure and Health Profile. EJBI 2020; 16(2): 22-28. DOI: 10.24105/ejbfi.2020.16.2.22
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact submissions@ejbi.org
Abstract
Objectives: There is a worldwide increase in the rate of obesity and its related long-term conditions, emphasizing an immediate need to address this modern-age global epidemic of healthy living. Moreover, healthcare spending on long-term or chronic care conditions such as obesity is increasing to the point that requires effective interventions and advancements to reduce the burden of healthcare.
Methods: This research focuses on developing a mobile application for obesity risk assessment using wearable technology and proposing an individualized activity/dietary plan. From calculating the Body Mass Index, we established an individualized health profile and used the average data collected by a smart vest to offer the level of activity and health goals.
Results: We developed an algorithm to assess the risk of obesity using the individual’s current activity and calorie expenditure. The algorithm was deployed on a smartphone application to collect data from the wearable vest and user-reported data. Based on the collected data, the proposed application assessed the risk of obesity/ overweight, measured the current activity level and recommended an optimized calorie plan.
Conclusion: The proposed model can integrate data from multiple sources including sensors, wearable garment, medical devices and also the manually entered (user reported) data. The model (and its rule-based engine) will continuously self-learn and tune the model for better accuracy and reliability over-time.
Keywords
Obesity risk assessment; Mobile health; Wearable technology; mHealth; Activity detection; Smartphone applicationmethods; Diabetes; Self-management
Introduction
This paper is an extension of work originally presented in personalized health (pHealth) 2019 on obesity risk assessment model using personalized activity, calorie expenditure and health profile [1]. Assessment, treatment, and management of obesity have become a major concern for governing bodies and healthcare organizations [2,3]. Many initiatives are focusing on prevention and early detection of health conditions, including chronic illnesses and long-term conditions (LTCs). The LTCs can be related to several health conditions such as diabetes, obesity and heart disease [4,5]. Currently, there is a need for a reliable and accurate application to determine the individual’s health profile from various data points such as activity data, vital signs, calories intake and self-reported data.
Obesity is a medical condition where individuals have excessive body fat that ultimately has adverse effects on their health. It is caused by two significant factors: excessive caloric intake and minimal physical activity [6]. Obesity contributes to various health conditions such as heart disease, Type 2 diabetes and many other chronic diseases, all of which reduce healthy living and life expectancy [6-8].
Short-term interventions, which are typically three to six months in duration, have examined the effect of exercise alone and in combination with reductions in energy intake on changes in body weight. When compared, these studies have demonstrated that reductions in energy intake (e.g., diet) have a greater impact on body weight than changes in energy expenditure via exercise, with the combination of diet plus exercise having the greatest impact on weight loss [9-11].
This research focuses on the early detection and individualized risk assessment for obesity using a proposed health profile concept. We developed an algorithm that identifies the individual’s level of the activity using activity data, vital signs and calorie intake (self-reported). The development of the algorithm involved using MATLAB and Microsoft Visual Studio environment. The wearable device used in this research was Hexoskin’s smart vest [12], that has the capability of measuring ECG, heart rate, heart rate variability, breathing rate, breathing volume, activity, steps and cadence in real-time and store the data in the cloud for further data analysis [12-15].
Data Collection and Preprocessing
Measured Variables
The following six key variables were measured for identifying the level of individual health [16-18].
• Daily Caloric Expenditure (DCE): Measured in Calories and is related to the activity level of an individual.
• Caloric Intake: A key measure of calories consumed for weight management. This is based on the standard calory intake per day for male and female.
• Breathing Rate: Measured in bpm and identifies the breathing rate. For people with LTCs such as obesity, breathing rate tends to be on a higher side (when compared to the healthy population).
• Real-time Electrocardiogram (ECG): This data is an effective measure for determining cardiovascular and heart-related issues.
• Minute Ventilation: Measures the volume of air that is inhaled or exhaled. It is measured in ml/min.
• Cadence: It is a measure of how many steps someone takes per minute (spm). Integrating this measurement will give the total steps someone takes over the recorded period.
Data Collection
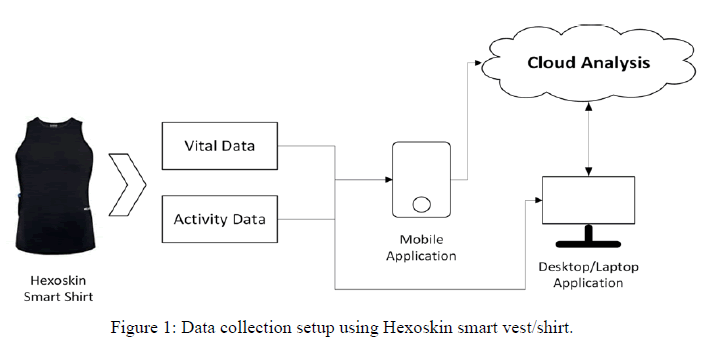
Data collection began by wearing the Hexoskin’s smart vest for a week, which measured many useful health parameters such as heart rate, breathing rate, cadence, minute ventilation and activity level. Initially, three male students between 21 to 23 years old involved in the project were recruited as a group of volunteers. However, over the research and developing period, the model and its rule-based engine will use the new data to continuously selflearn and tune the model for better accuracy and reliability. Using Hexoskin’s smart vest, we collected real-time activity (cadence), ECG, heart rate, breathing rate and minute ventilation. Figure 1 shows the setup of data collection using the Hexoskin smart vest and its related application programming interfaces (APIs) as well as a cloud platform. The collected data stored on the Hexoskin’s cloud platform with full access to the data via its open APIs. The wearable smart vest data can be collected from the cloud platform, and each measured variable can be extracted in its processed and raw formats. We extracted the raw data related to the selected variables in real-time using the Hexoskin APIs and saved them to a .csv file.
In addition to the data collected by Hexoskin vest, the Body Mass Index (BMI) is measured to classify the users in different categories. BMI is one of the key indicators of body fat and is defined as the body mass divided by the square of the body height by the American Heart Foundation. BMI intends to classify an individual into different categories, from underweight to obese [19-21]. BMI can only be considered as a rough estimate for obesity condition of a person. BMI is not a sophisticated measure to determine or differentiate the finer details regarding age, body fat, muscle mass, fat mass and bone mass. Hence, BMI by itself cannot be a reliable metric to quantify the health of a person in this scenario. So, taking the inaccuracy of BMI into account, the average Hexoskin smart vest data, as described in Sections 2.2 and 2.3, were considered in the algorithm to analyze the user-health condition.
Preprocessing of Data
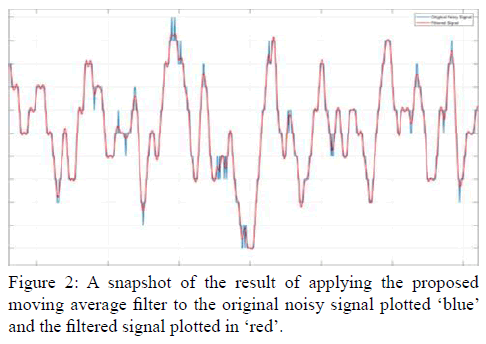
Pre-processing of wearable sensor data was identified as a challenging task due to the motion artifacts and time/ frequencyrelated noises associated with each sensor/variable. Thus, it was critical to reduce the noise in the signals received and normalize the incoming data for uniqueness. A moving average filter was applied to the whole dataset for denoising data by taking a certain number of samples (window) across a given period and taking the average of the sample values as an output. This window moved across the data and produced a series of average, which then made up the output of the moving average filter. An example of smoothing the data is presented in Figure 2 with original noisy signal plotted in ‘blue’ and the filtered data plotted in ‘red’.
The reason for taking the raw data was to implement an improved smoothing low pass filter to remove outliers caused by the sensor picking up noise, as shown in Figure 3.
The filter that employed to remove the noise introduces a delay in the signal. The order of the selected low pass filter was six. Therefore, each output sample was calculated as a weighted sum of the last six input samples. The filtering algorithm was implemented using Visual Studios.
Methodology
Data flow is a key aspect that allows the successful execution of the app. So initially, data is collected from the Hexoskin smart vest and passed to the phone via Bluetooth. This connectivity is only accessed using the original Hexoskin API. The user then sinks the data on the phone with the online Hexoskin API server. This data is stored in a CSV file on the server. Within our app, the latest CSV file can be retrieved from the Hexoskin API. A MATLAB executable file is then run by the app to process the data and receive the average values for each parameter monitored by the Hexoskin vest. These average values on MATLAB are also used to calculate the overall scale value. These calculated values are passed back to the app for display and for assigning which plans will be shown to the user. In addition to the data collected by Hexoskin vest, the BMI is calculated to establish the individual health profile.
We used BMI to categorize the user in one of the four standard categories from underweight to obese (Table 1) and then considered the average Hexoskin smart vest data to select a dietary/activity plan for the user.
| Obesity Class | BMI Range |
|---|---|
| Underweight | <18.5 |
| Healthy | 18.5-24.9 |
| Overweight | 25-29.9 |
| Obese | ≥ 30 |
Table 1: Obesity classification according to the World Health Organization guidelines.
Daily Caloric Expenditure and the Harris-Benedict Equation
The DCE is an estimation of how many calories expended by an individual per day which is related to the amount of energy required to maintain the body‘s normal metabolic activity at rest with no additional activity or Basal metabolic rate (BMR). This factor is related to the Harris-Benedict equation that expresses the DCE by multiplying the BMR and an activity multiplier (Global RPh) (22).
Male (metric): DCE = ALF x ((13.75 x WKG) + (5 x HC) - (6.76 x age) + 66) (1)
Female (metric): DCE = ALF x ((9.56 x WKG) + (1.85 x HC) - 4.68 x age) + 655) ) (2)
Where ALF is Activity Level Factor, WKG is weight in kilograms and HC is height in centimeters.
Quantifying Health of Individuals
The essential part of the risk assessment model is to design and develop an accurate individualized scale by which the health of an individual can be deduced. We used the weight parameter mechanism using three data types - Activity data, vital signs and calorie intake. The weighted parameters are shown in Table 2, which are based on the DCE distribution [19,22-24].
| Name | Class | Weight |
|---|---|---|
| BMI | A | 50% |
| Heart Rate | B | 12.50% |
| Breathing Rate | C | 12.50% |
| Minute Ventilation | D | 12.50% |
| Caloric Expenditure | E | 12.50% |
Table 2: Weighted scales of the individual health parameter.
Most risk models use BMI as the only measure to profile atrisk individuals. However, the proposed model assigns a higher weight to BMI due to its impact on the overall risk profile, but the model also considers other data sources such as data received from the wearable monitoring (Hexoskin [12]) to establish an accurate health risk profile as the “Overall scale”.
Algorithm Development
Initially, each variable (ECG, heart rate, cadence, calories, breathing rate and minute ventilation) was normalized with its standard limits using the best-practice and national guidelines. Moreover, an individual scale was established for each variable and then the overall scale was developed. The standard heart rate ranges were used to establish the individual’s range, maximum and minimum values. Table 2 shows the class and weight of each variable, derived from the DCE distribution. For each variable, an individual scale (ranging from 0 to 100) is created based on its corresponding range. Then, the overall scale was established using the weights from the individual scale and its respective categories (equation 3). Table 1 provides the final parameters of each category [23,25-27].
Overall Measure = A*0.5+B*0.125+C*0.125+D*0.125+E*0.125 (3)
Where, A = (average BMI value)/40*100, B = (average heart rate value)/220*100,
C = (average breathing rate value)/50*100, D = (average minute ventilation value)/60*100, and
E = 100 – (calculated calorie value)/10,000*100
Mobile App (Prototype) Development
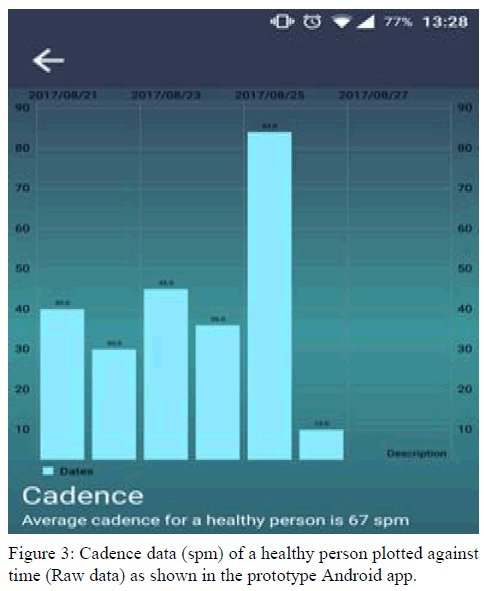
The proposed scaling scheme applied to the data collected from the Hexoskin’s smart vest. The scale value is a number ranging from 0 to 100 where the value around 50 is termed as a healthy region. The range value of less than 50 is categorized as underweight and anorexic, and the range value above 50 is categorized as overweight and obese. Finally, the scale’s index value was stored on a cloud server, which was then received by the app and displayed to the user. Based on the scale value, the app displays different workout regiments and dietary plans to ensure that the user reaches the desired healthy region. A sample screen with cadence data from the prototype Android app is shown in Figure 3.
A list of features (menu) that users can interact with the prototype app is overview, analysis, plan, user profile and help. The ‘Overview’ is the main menu that users can see once logged into the app. The menu contains most of the user info where the scale value was retrieved from the cloud database. The scale value determines the user’s health. The ‘Overview’ also shows the daily averages of the user’s data which includes heart rate, breathing rate, cadence, and minute ventilation. It will also show the user’s current workout routine and the current meal that the user is recommended to take.
In the ‘Analysis’ tab, the user‘s health parameters are displayed. It shows a bar graph with the averages within the week. Below the graphs, are the averages for that parameter with a healthy range so the user can compare the results with a healthy range. The ‘User Profile’ shows the user details submitted at the time of sign up. It includes name, email address, age, height and weight. In the ‘Help’ tab, we described some key terms used within the app, for example ‘cadence’. It also shows how the healthy range is defined so it is easy to know and understand the whole scale and its interpretation for anorexic or obese range. The equation used to define the algorithm can also be found in the help section of the application.
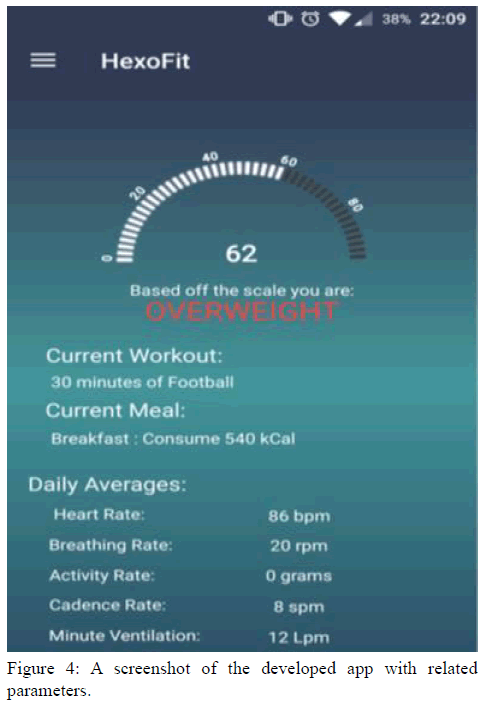
Figure 4 shows a screenshot of the developed app where the layout consists of primarily text boxes which present useful information related to the health profile, activities and dietary plan.
Data Protection and Privacy
Firebase was employed as a cloud storage application to store an individual’s data virtually. It is a well-established platform where different mobile applications have used it for data protection and security purposes. The other features of Firebase include real-time, authentication, cloud storage, crash reporting and many more. In this work, the authentication function was used to allow users to have the ability to login into the app using their secure login and password. Having a login identification allows individuals to have access to their private data and serves as a common functionality like the pre-existing Hexoskin app.
Results and Validation
In order to ensure that the proposed algorithm can accurately identify the health category of a person, a testing dataset was needed. Instead of finding data on an actual population with the specific variables needed for input into the algorithm, a simple procedure was used to simulate an actual population sample. A set of 100 random numbers were generated for each variable including Age, Height and Weight. For each variable, the generated numbers were limited to be within a specific range. For example, the age was limited within a range of 18 to 100. For example, an individual cannot have a BMI of less than 12 and thus, certain limits were introduced to ensure that all data in the sample was valid. Form the sample generated BMI, DCE for females, DCE for males and values for the overall scale were calculated [28].
The BMI distribution of the simulated compared with the “Public Health of England” [29,30]. Since DCE only approximates a recommended daily caloric intake for maintaining user’s current weight, it cannot be used as the actual recommended intake for people who are below or above the healthy range. Thus, the result of the overall health scale was used to determine a factor by which the calculated DCE is multiplied. The multiplying factors are derived from the male and female DCE distribution on a large population data from the national health survey [29-33]. Table 3 shows the derived multiplying factors for calculating DCT for different categories of obesity.
| Obesity Class | Multiplying Factor |
|---|---|
| Underweight | 1.5 |
| Healthy | 1 |
| Overweight | 0.75 |
| Obese | 0.5 |
Table 3: Multiplying factors derived from the population data.
Using the DCE distribution results, 10 DCE sub-ranges were established. Within each category, there are three sets of daily plans and each plan is limited in calories based on the range. Each plan aims to support the individual to achieve a healthy target and stay on a path to attain their individual health goals. An example of one of the plans includes Breakfast, Morning Snack, Lunch and Dinner consisted of 30%, 15%, 30% and 25% of the daily calories limit respectively [25-27,31-33].
To extend the proposed algorithm for dietary and exercise recommendation, we adopted multiple platforms such as Visual studios, MATLAB, Firebase and Android Studios for the development and the deployment of the prototype application. Through this research, the current state of health of the user can be determined, thus allowing for remote health monitoring. Data collection and analysis was successfully implemented using a mobile app which displays the user’s health profile through an algorithm formulated from the parameters measured by Hexoskin’s smart vest [12]. The data was then passed through the mobile app developed on Android Studio which recommends the user with dietary and workout plans formulated to cater to each division of the scale.
To validate the proposed model, we employed a group of volunteers to wear the Hexoskin smart vest and record the required data. The outliers were removed using an automated outlier detection module, and the generated data was robust enough to cover all possible scenarios and categories. The data was securely stored on the cloud platform in real-time for data analysis and data mining. We used the Hexoskin’s open APIs to load the real-time data into our local environment for pre-processing and risk analysis. By running the MATLABTM executable file on the app and process the data, the average values for each of the variables monitored by the Hexoskin suit were calculated [12]. The average values were used to calculate the overall scale using the local MATLABTM environment. These calculated values are passed back to the online application for the display of information and also for assigning the individual’s calorie plans. The user will see the individualised calorie plan, health profile (activity status and vital signs) and the overall risk of obesity.
Conclusion and Future Work
The collected data is mapped against the pre-built overweight and obesity model and approved clinical guidelines. The proposed model can integrate data from multiple sources including sensors, wearable garment, medical devices and also the manually entered (user reported) data. The model (and its rule-based engine) will continuously self-learn and tune the model for better accuracy and reliability over some time. An intelligent model to analyze the obesity levels in adults is represented by a prototype Android app. It allows users to login with their data which is first collected from Hexoskin’s smart vest and then uploaded to the app after processing the data. An added benefit is the ability to provide the user with a dietary plan and workout program catered to each category and defined on the scale going from anorexic to obese. Each plan is prepared with the calories of each meal, and the workout states the number of calories the users can lose if working out with that specific activity and duration of the exercise.
Future work will involve the addition of more sensors to measure other parameters such as body temperature and oxygen saturation; enhancing the real-time capability as the app currently updates the user’s data every twenty-four hours. The design of the user interface could also be enhanced by improving the overall aesthetics of the design as well as adding more functionalities to each screen. This would allow the user to have more freedom in understanding their data as well as learning more about their health and activities through informative analysis. To further provide the user with information, a website could be developed to share more information with the user, for example, a more detailed graph which may display a peak on how active the user was on that day and showing what time, they did that activity. Another future development for the app would be taking the design to the next level using a cross-platform approach such as React Native for IOS users as currently, the app is only available for Android users. One other option for the application of this health monitoring app could be to act as a standalone fitness app. Currently, it is running in conjunction with Hexoskin’s app and database but it could later be programmed to use with other heart monitoring or breathing monitoring sensors such as a Fitbit.
Acknowledgment
We would like to thank Hexoskin for supporting this research by providing the advanced wearable vests (smart vest), access to the mobile app and cloud platform with APIs, which are used for the real-time data collection in this research project.
Conflict of Interest
Authors declare no conflict of interest.
REFERENCES
- Gholamhosseini H, Baig M, Maratas J, Mirza F, Lindén M. Obesity Risk Assessment Model Using Wearable Technology with Personalized Activity, Calorie Expenditure and Health Profile. Studies HTI. 2019; 261: 91-6.
- Pearl RL, Wadden TA, Hopkins CM, Shaw JA, Hayes MR, Bakizada ZM, et al. Association between weight bias internalization and metabolic syndrome among treatment‐seeking individuals with obesity. Obesity. 2017; 25(2): 317-22.
- Puhl RM, Himmelstein MS, Quinn DM. Internalizing weight stigma: prevalence and sociodemographic considerations in US adults. Obesity. 2018; 26(1): 167-75.
- Thornicroft G, Ahuja S, Barber S, Chisholm D, Collins PY, Docrat S, et al. Integrated care for people with long-term mental and physical health conditions in low-income and middle-income countries. The Lan Psych. 2018.
- Potter CM, Kelly L, Hunter C, Fitzpatrick R, Peters M. The context of coping: a qualitative exploration of underlying inequalities that influence health services support for people living with long term conditions. Sociology of Health & Illness. 2018; 40(1): 130-45.
- Xie L, Su H, Sun C, Zheng X, Chen W. Recent advances in understanding the anti-obesity activity of anthocyanins and their biosynthesis in microorganisms. Trends Food Sci Tech. 2018;72:13-24.
- Xu F, Cohen SA, Lofgren IE, Greene G, Delmonico MJ, Greaney ML. The Association between Physical Activity and Metabolic Syndrome in Older Adults with Obesity. JFA. 2019;8(1):27-32.
- Lambert GW, Schlaich MP, Eikelis N, Lambert EA. Sympathetic activity in obesity: a brief review of methods and supportive data. Ann NY Acad Sci. 2019.
- Innerd P, Harrison R, Coulson M. Using open source accelerometer analysis to assess physical activity and sedentary behaviour in overweight and obese adults. BMC Public Health. 2018; 18(1): 543.
- Huffman LE, Wilson DK, Van Horn ML, Pate RR. Associations between parenting factors, motivation, and physical activity in overweight African American adolescents. Annals of Behavioral Medicine. 2018; 52(2): 93-105.
- Sherar L, Mirwald R, Erlandson M, Baxter-Jones A. Is boys’ physical activity in childhood associated with being overweight in mid-adulthood? A longitudinal study spanning 35 years. Canadian Studies in Population. 2018; 34(1): 85-99.
- https://www.hexoskin.com/
- Smith CM, Chillrud SN, Jack DW, Kinney P, Yang Q, Layton AM. Laboratory Validation of Hexoskin Biometric Shirt at Rest, Submaximal Exercise, and Maximal Exercise While Riding a Stationary Bicycle. JOEM. 2019; 61(4): e104-e11.
- Elliot CA, Hamlin MJ, Lizamore CA. Validity and reliability of the Hexoskin wearable biometric vest during maximal aerobic power testing in elite cyclists. J Strength Cond Res. 2019; 33(5): 1437-44.
- Moriarty TA, Feito Y, Monahan J, Williamson C. Using the Hexoskin Smart Garment to Measure Cardiorespiratory Variables During High Intensity Functional Training: 2760 Board# 43 June 1 200 PM-330 PM. Medicine & Science in Sports & Exercise. 2018; 50(5S): 673.
- Seaton CL, Holm N, Bottorff JL, Jones-Bricker M, Errey S, Caperchione CM, et al. Factors that impact the success of interorganizational health promotion collaborations: a scoping review. AJHP. 2018; 32(4): 1095-109.
- Seguin RA, Paul L, Folta SC, Nelson ME, Strogatz D, Graham ML, et al. Strong Hearts, Healthy Communities: a community‐based randomized trial for rural women. Obesity. 2018; 26(5): 845-53.
- Chin M-K, Edginton CR, Tang M-S, Phua K-W, Yang J-Z. School and Community-Based Physical Education and Healthy Active Living Programs: Holistic Practices in Hong Kong, Singapore, and the United States. Global Perspectives on Childhood Obesity: Elsevier; 2019. p. 325-37.
- Henry C. Basal metabolic rate studies in humans: measurement and development of new equations. Public Health Nutrition. 2005; 8(7a): 1133-52.
- Leung J, Ridley EJ, Cleland H, Ihle JF, Paul E, King SJ. Predictive energy equations are inaccurate for determining energy expenditure in adult burn injury: a retrospective observational study. ANZ Journal of Surgery. 2019; 89(5): 578-83.
- Tabata S, Kinoshita N, Yamada S, Matsumoto H. Accuracy of basal metabolic rate estimated by predictive equations in Japanese with type 2 diabetes. Asia Pacific J Clin Nutr. 2018; 27(4): 763.
- Roza AM, Shizgal HM. The Harris Benedict equation reevaluated: resting energy requirements and the body cell mass. Am J Clin Nutr. 1984; 40(1): 168-82.
- Jensen MK, Chiuve SE, Rimm EB, Dethlefsen C, Tjonneland A, Joensen AM, et al. Obesity, behavioral lifestyle factors, and risk of acute coronary events. Circulation. 2008; 117(24): 3062.
- Ryan M, Yi D, Avenell A, Douglas F, Aucott L, Van Teijlingen E, et al. Gaining pounds by losing pounds: preferences for lifestyle interventions to reduce obesity. Health Economics, Policy and Law. 2015; 10(2): 161-82.
- Pearl RL, Puhl RM. Weight bias internalization and health: a systematic review. Obesity Reviews. 2018; 19(8): 1141-63.
- Batsis JA, Whiteman KL, Lohman MC, Scherer EA, Bartels SJ. Body Mass Index and Rural Status on Self‐Reported Health in Older Adults: 2004‐2013 Medicare Expenditure Panel Survey. The Journal of Rural Health. 2018; 34: s56-s64.
- Duncan L, Georgiades K, Wang L, Comeau J, Ferro MA, Van Lieshout RJ, et al. The 2014 Ontario Child Health Study Emotional Behavioural Scales (OCHS-EBS) part I: a checklist for dimensional measurement of selected DSM-5 disorders. The Canadian Journal of Psychiatry. 2019; 64(6): 423-33.
- Lim JU, Lee JH, Kim JS, Hwang YI, Kim T-H, Lim SY, et al. Comparison of World Health Organization and Asia-Pacific body mass index classifications in COPD patients. Int J Chron Obstruct Pulmon Dis. 2017; 12: 2465-75.
- Wang YC, McPherson K, Marsh T, Gortmaker SL, Brown M. Health and economic burden of the projected obesity trends in the USA and the UK. The Lancet. 2011; 378(9793): 815-25.
- Green M, Subramanian S, Razak F. Population-level trends in the distribution of body mass index in England, 1992–2013. J Epidemiol Community Health. 2016; 70(8): 832-5.
- Mariapun J, Ng C-W, Hairi NN. The gradual shift of overweight, obesity, and abdominal obesity towards the poor in a multi-ethnic developing country: findings from the Malaysian National Health and Morbidity Surveys. Journal of Epidemiology. 2018: JE20170001.
- Thomas A, Janusek L. Obesity Prevention Behaviors in Asian Indian Adolescent Girls: A Pilot Study. Journal of Pediatric Nursing. 2018; 42: 9-15.
- Breslau J, Stein BD, Han B, Shelton S, Yu H. Impact of the Affordable Care Act’s dependent coverage expansion on the health care and health status of young adults: what do we know so far? Medical Care Research and Review. 2018; 75(2): 131-52.